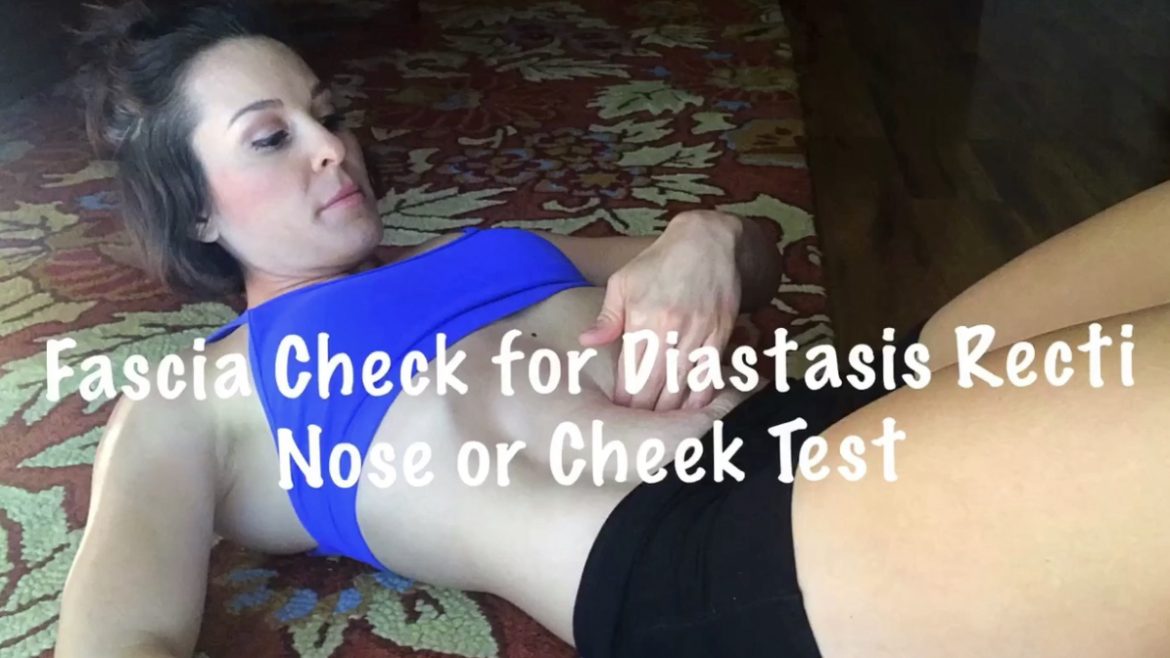
I get asked these two questions almost daily. “Have you closed your gap?” and “How do I close my gap?” My short answer is “sort of,” and “it doesn’t entirely matter.”
Here is the longer answer…
My experience in “healing” my core.
You can read my more in-depth story here. I started with a 4-finger gap and fascia that you could press your fingers into at least middle-knuckle deep. After 7 and 6 pound twins, a lifetime of less than ideal posture and body mechanics, and a history of overtraining my rectus abdominis (the six-pack muscles), and unknowingly neglecting the transverse abdominis (the inner-most abs that act like a corset), I had the perfect storm for a hefty abdominal separation.
At about six months postpartum, realizing that my stomach looked continually “poochy,” I discovered my diastasis recti and proceeded to find a pretty awesome pelvic floor physical therapist who started me on my journey to heal.


Find a pelvic floor physical therapist in your area by zip code!
Where am I at now?
It has been a hard fought journey to get my core strength to what it is today. I still measure about 2-fingers wide, but my fascia has much improved. Relaxed, I can get slightly deeper than the base of my finger nails. But here is the real measure of success—if I engage my core by using my core/pelvic floor breath, I can get a pretty taught fascia. Perfect? Nope. Strong? Yep.
Why the width of the gap isn’t all that significant.
I’m not going to recreate the wheel here. Lorraine Scans from Pregnancy Exercise in New Zealand does a wonderful job summarizing research by the industry revolutionary Diane Lee. Give it a read! And if you want Diane Lee’s more academic version, check it out.
The general idea is that being able to gain tensile strength…nice, taught fascia is an incredibly important factor in measuring healing. The gap might exist indefinitely, but you are “healed” if you can get that fascia that connects the six-pack muscles firing.
Diane says healing occurs when one is able, “…to achieve optimal strategies for transferring loads through the abdominal canister.” She continues asking if the patient can function, “In multiple vertical loading tasks (single leg standing, squatting, walking, moving from sit to stand, and climbing stairs).” If the fascia isn’t firing, the “load transfer through the pelvic girdle and/or hip joint is consistently found.”
Simply put, if your fascia isn’t firing, whether you have a gap or not, your body will compensate with less than ideal strategies, resulting in lower back pain, pelvic floor dysfunction, hip pain, and more.


Read up, and watch the video below to check yourself!